MCRs in the Community
Announcing New MCR Territory Coverage Assignments
by Jennifer Borrillo, Senior Vice President Member & Community Relations
Ashley Castello, Jazzmine Brown, and Kelly Waters joined the Hemophilia Alliance team in September as new Directors of Member & Community Relations. These new additions reflect both expansion and transition within the team—one new position, one to succeed Jeff Amond, who recently left the Alliance, and one to follow Mark Plencner, who will be retiring in January of 2026.
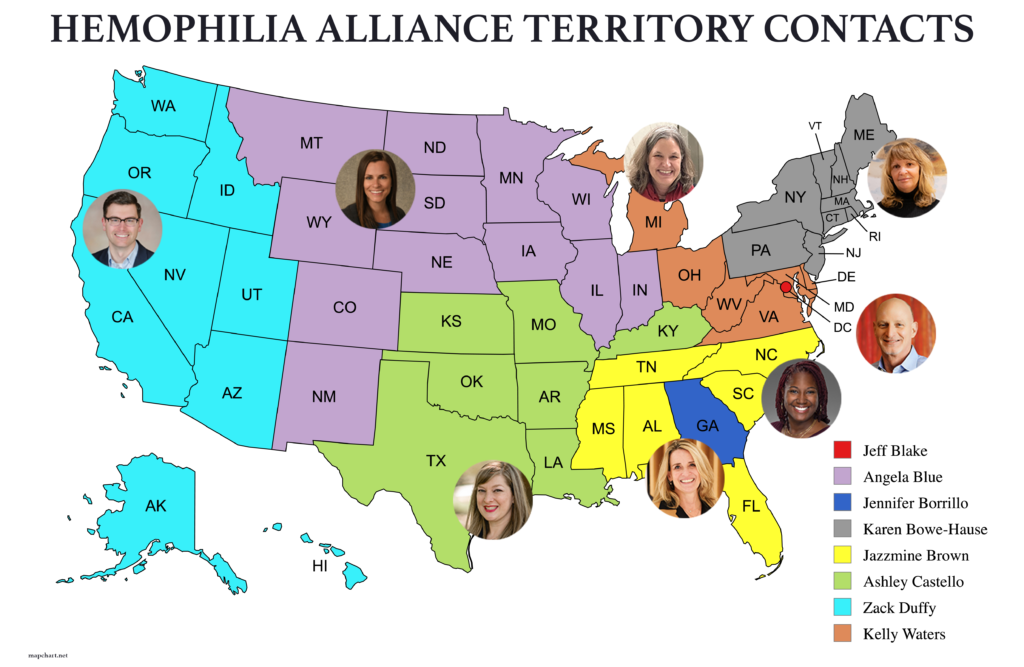
At the Fall Member Meeting held in Washington, DC on September 6, 2025, the updated MCR Territory Map was shared with attendees and those in attendance were able to meet Ashley, Jazzmine, and Kelly in person. The entire Hemophilia Alliance team, and the MCRs in particular have worked so closely with our member HTCs, and are sensitive to the uncertainty change brings, no matter how exciting it can be. Angie, Mark, Karen, Zack, and Jennifer will still be working with each of their previously assigned HTCs throughout the remainder of 2025, while also personally introducing Ashley, Jazzmine, and Kelly to the HTCs they will become the primary MCR contact for in 2026.
Your primary MCR is your first point of contact for Hemophilia Alliance communications. Your assigned primary MCR contact will triage your questions and issues, help assess next steps, assist with strategic discussions, and help with planning for the future. The MCRs are a small but mighty team that quickly pulls in other team members to provide guidance and/or to resolve issues as needed. Remember to notify your MCR contact as soon as you have a question or an issue arises. Reaching out to the MCR team proactively allows for early intervention and helps the MCR team to better address issues in a timely manner. If you are running into an issue, it is likely that another HTC is running into a similar issue.
We cannot stress enough that there are no “stupid” questions, so please reach out to your primary HTC MCR contact with any questions you may have. We are here to help you navigate those questions and find the answers, viable solutions, and resources needed. Remember, we work for you!
| Name | Phone | |
|---|---|---|
| Jennifer Borrillo, MSW, LCSW, MBA | borrillo@hemoalliance.org | 504-376-5282 |
| Angela Blue, MBA | angela@hemoalliance.org | 651-308-3902 |
| Karen Bowe-Hause, MBA, MT | karen@hemoalliance.org | 717-571-0266 |
| Zack Duffy, MBA | zack@hemoalliance.org | 503-804-2581 |
| Mark Plencner | mark@hemoalliance.org | 701-318-2910 |
| Ashley Castello, M.Ed. | ashley@hemoalliance.org | 225-266-5062 |
| Jazzmine Brown, MBA, MSW, LCSW | jazzmine@hemoalliance.org | 770-570-2649 |
| Kelly Waters, MSW. LCSW | kelly@hemoalliance.org | 804-317-4998 |
| Kollet Koulianos, MBA | kollet@hemoalliance.org | 309-397-8431 |
| Roland P. Lamy, Jr. | roland@hemoalliance.org | 603-491-0853 |
| Dr. George L. Oestreich, Pharm.D., MPA | george@hemoalliance.org | 573-230-7075 |
Building Connections and Navigating Change in Medicaid Leadership
by George Oestreich, Government Payer Consultant Hemophilia Alliance
Staying connected with your state Medicaid leadership is more important than ever. For Hemophilia Treatment Centers (HTCs), building relationships with your state’s Medicaid director and pharmacy program staff can make a real difference in shaping policies and reimbursement processes that affect patient care. Recent discussions among the National Association of Medicaid Directors Alumni Group have highlighted new challenges and opportunities, especially as Medicaid program leadership changes continue across the country.
Who’s New? Medicaid Director Transitions
There’s been a wave of new appointments and interim directors in Medicaid programs nationwide. Here are some of the latest changes:
- Idaho: Sasha O’Connell is now leading, succeeding Juliet Charron.
- Illinois: Laura Phelan has taken over from Kelly Cunningham.
- Wyoming: Jesse Springer is serving as interim director, following Lee Grossman.
- Iowa: Lee Grossman is now director, succeeding interim Rebecca Curtis.
- Louisiana: Drew Maranto is interim director, succeeding Kim Sullivan.
- Maryland: Perrie Briskin has replaced Ryan Moran.
- Nevada: Ann Jensen is now director, succeeding Stacie Weeks.
- Vermont: Ashley Berliner is interim director, following Jill Olson.
- Utah: Nate Checketts is interim director, succeeding Jen Strohecker.
- Puerto Rico: Luz Cruz is interim director, succeeding Carlos Santiago-Rosario.
- Ohio, Missouri, New Mexico: New directors are yet to be determined.
These transitions mean that many states are adjusting to new leadership styles and priorities. For those working with Medicaid, it’s a good time to review your contacts and consider reaching out to introduce yourself or reconnect.
Facing Today’s Challenges
Medicaid directors are dealing with tough challenges, including budget constraints and operational disruptions. Reduced federal revenue and the lack of reserve accounts in some states are putting extra pressure on agencies. Many directors are navigating budget downturns for the first time, making peer support and shared best practices more valuable than ever. Without HTC input, the agencies will not know how the new landscape will impact your ability to efficiently manage your patient’s bleeding disorders, which are known to be expensive to treat.
In summary: The landscape of Medicaid leadership is changing rapidly, and HTCs, who work with Medicaid programs, can play a vital role by building relationships, offering support, and staying informed about new developments. It is imperative for you to help your state’s Medicaid program understand how these changes can help you better serve Medicaid-eligible patients and contribute to positive value-added outcomes.
Open Enrollment is Upon Us: BEWARE OF JUNK HEALTHPLANS
by Kollet Koulianos, Senior Payer Consultant Hemophilia Alliance
As healthcare open enrollment nears, it’s essential for our HTCs to inform patients who are buying their own insurance (outside of employer-sponsored plans) about the dangers of “junk health plans.” These plans often provide limited coverage and can leave patients with significant out-of-pocket costs. Junk plans are expected to be more common this year, except in the 12 states and Washington, D.C., that have passed laws banning their sale. However, even in those states, certain junk plains (such as Christian ministry plans and Farm Bureau plans) are still allowed to be sold. These plans aren’t classified as insurance but often function as what we consider “junk plans,” especially for those with chronic health conditions.
These plans are often appealing because of their affordability but come with major red flags: limited provider networks, no prescription drug coverage, and exclusions for pre-existing conditions or high-cost specialty medications. For people living with diseases like hemophilia, multiple sclerosis, diabetes, or cancer, those gaps aren’t just inconveniences—they’re life-threatening.
Chronic disease care requires consistency, coordination, and access—not fine print. Before enrolling, patients should verify that a plan covers their prescribed medications, make sure their specialists are in-network, and the plan complies with Affordable Care Act protections.
How Our Patients Can Identify Junk Health Plans
1. Look for the Fine Print
If a plan doesn’t comply with Affordable Care Act (ACA) requirements—such as covering essential benefits—it’s not true comprehensive insurance. Signs might include:
- Excluding preexisting conditions or limiting annual payouts.
- Not covering specialty medications
- Being described as “temporary,” a “bridge plan,” “health sharing,” or “fixed indemnity”
- Capping coverage, requiring large upfront payments, or refusing to cover your medications of specialists
- Make sure your specialist and/or treatment center is actually in network. Some junk plans claim you can “see any doctor,” but offer little to no reimbursement for those visits
2. Red Flags to Watch For
Be cautious if a plan shows any of these warning signs:
- Not available on Healthcare.gov
- Marketed through social media ads or robocalls
- Sold by “benefit associations” or “faith-based” groups rather than licensed insurers
For chronic conditions, prescription coverage is crucial, watch for:
- “Discount cards” instead of real prescription coverage
- Exclusion of specialty medication
- Use of “alternative funding” schemes that require you to apply for copay assistance instead of using your insurance benefits
Remember: Only ACA-compliant plans sold through legitimate state or federal marketplaces guarantee essential health benefits and consumer protection.
3. Trust Your Instincts
If the deal seems too good to be true (such as $200/month for “comprehensive” coverage) it almost always is.
Bottom Line
Real health plans protect you when you need care the most. Junk plans protect insurers’ profits instead. Before enrolling, check with:
- Healthcare.gov
- Your state insurance department
- Reach out to your MCR team member at the Hemophilia Alliance.
Because when it comes to chronic disease, a “cheap” plan can become the most expensive decision of your life.
We’d love your input on future newsletter topics
Also In This Issue…
Jeff Weighs In
Washington Update
- Government Shutdown Begins – and Continues
- Alliance Hill Day
- 340B Legislation and Hearing
Administration and Operations Update
- No Tricks, Just Impact: Fall Meeting Highlights